Who knew something as small as your big toe could cause so much agony. Bunions are incredibly common and can be incredibly painful. One study from the Journal of Foot and Ankle Research estimates that roughly 36 percent of adults over 65-years-old suffer from bunions. While common, many people do not know as much as they should about bunion care, including the most important thing, how to deal with them. Dr. Michael Dujela is a board certified, orthopaedic-fellowship-trained podiatric foot and ankle surgeon at Washington Orthopaedic Center, located in Tumwater and Centralia. He sees a lot of bunion cases at his practice. Because of his commitment to his patients, he wants to share his knowledge to help people be more informed about this common foot problem.

When he is not caring for patients, Dujela is traveling the world giving talks and teaching other surgeons in his field. He is the immediate past national chairman of the Education and Scientific Affairs Committee for the American College of Foot and Ankle Surgeons, the professional organization that develops surgical courses and materials. Dujela recently co-authored a chapter on recurrent bunion deformities for a textbook titled Evidence-Based Bunion Surgery: a critical examination of current and emerging concepts and techniques.
If you have a bunion, you should know that every person is different. What is causing yours is not the same as everyone else. Going to a doctor that will treat you as an individual case is important, to ensure you get the right treatment. “One thing that Dr. Dujela does that stands out is patient-centered care,” says Ali Peterson, operating room charge nurse. “He really pays attention to what each person needs in the operating room. He is there with them in pre-op, and is next to them when they are going under right before surgery.” This attention to his patients starts before the operating room, in the exam room, where he examines each individual case and what’s right for that patient right then.
Non-Surgical Methods for Living with Bunions
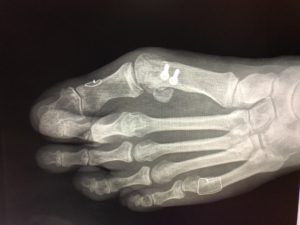
Photo courtesy: Washington Orthopaedic Center
Dujela often tries a period of non-surgical treatment before recommending surgery. He explains that while the structural deformity remains, these treatments can alleviate the pain and allow the patient to resume most of their normal activities. Depending on the patient, Dujela may recommend things like shoes with nice wide toe boxes, silicone padding, ice packs, anti-inflammatories, and activity modification.
“The reality is these people have had long standing deformity and what might have brought them in is not pain, but someone saying ‘hey what’s wrong with your foot?’” he shares. “So the referral is driven by a family member or a friend, but the patient is living quite reasonably with it. We only operate on the painful ones and/or ones that cause interruptions in your daily living.”
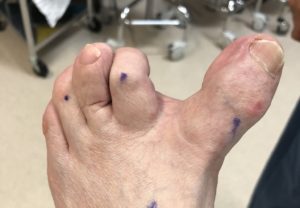
This doesn’t mean that it might not change down the road. Dujela sometimes sees patients up to 15 years later, that now need surgery because it’s causing them pain. But he isn’t going to do surgery unless it’s necessary. “If you are not having pain, how can we improve upon it?” he asks. “We do surgery for a functional outcome with a pleasant cosmetic result, not just for cosmetic reasons.”
When You Need Surgery
If the bunions are causing you pain or are interfering with your daily life, Dujela may recommend surgery at that point. It’s a highly complex procedure, even though it may only take the doctor 30 minutes to an hour-and-a-half to perform.
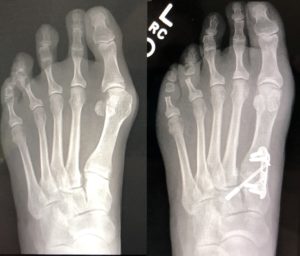
“We do the time-tested procedures, but we have continued to modify and improve them to get a much better functional result with a lower chance of recurrence,” Dujela explains, “because some patients and methods are prone to that.” Due to this, it’s extremely important to use the right method with the right patient. “The reality is that some of these operations are highly complex and take a tremendous amount of skill,” he adds, “and sometimes people may select a procedure they feel the patient may have an easier time recovering from, but may not give the best structural and functional outcome long term.”
Because bunions are caused by not only the toe joint shifting and rotating, but also the attached metarsal bone and it needs to be looked at as a 3-dimensional correction, not in one plane. Part of Dujela’s patient-centered care includes looking beyond the toe joint, to assess the patient’s entire foot, ankle and even the lower limb, including gait analysis. In some cases, they have poor alignment somewhere else in their foot or lower limb that is contributing to the overall problem. In these cases, if you just deal with the big toe joint, you are only correcting a symptom of a larger problem and the bunion may return, or a secondary problem may surface.
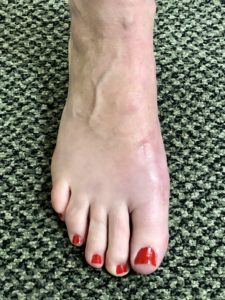
This is where Dujela’s experience is worth its weight in gold to his patients – he may choose a more complicated surgery that requires longer recovery, but you are less likely to have the bunion return or have other issues surface. Just how common are reoccurrences after surgery? If done properly, with the correct procedure for the patient’s needs, recurrence is rare. However, 10-15 percent of his cases are patients that come to him after having surgery somewhere else that did not correct the problem. Now, these patients face a more invasive surgery because he has to fix what was done before, as well as correct the secondary problems that may have surfaced.
If you are suffering from any kind of foot or ankle pain, it’s worth it to contact Dr. Dujela at Washington Orthopaedic Center. He will give you a full assessment of your individual case, answer your questions and give you a recommendation that is based on getting your body back to structurally sound and functional. Visit the Washington Orthopaedic Center website to learn more or call 800-342-02015.
Sponsored




















































