If you have no idea what an interventional radiologist does, you’re not alone. A study in Canada found that less than 6% of all patients had even heard the term before they were referred for a procedure, and 87% had no information on the subject. Until February, 2017, Cathy Obrien was among them.
But shortly before Valentine’s Day, she started having trouble swallowing. Doctors suspected an ulcer, but an endoscopy proved inconclusive so they planned more procedures to gather information. Before they could begin, Obrien started bleeding heavily from her GI tract and matters quickly became critical.

Across town, South Sound Radiology’s Dr. Alireza Bozorgmanesh, a.k.a. ‘Dr. Boz’, was having a pre-Valentine’s Day dinner with his wife when he got the call. He drove to the hospital where he was able to thread a tiny tube through an artery in Obrien’s left wrist and discover a large duodenal ulcer that was eating into the artery where the stomach becomes the small intestine. “He was able to send a very small coil up my arm, across, and into the bleeding area,” says Obrien. “It expanded and acted like a plug. My family and I believe his skill in stopping the bleeding saved my life. If this sub-specialty didn’t exist, I wouldn’t be here.”
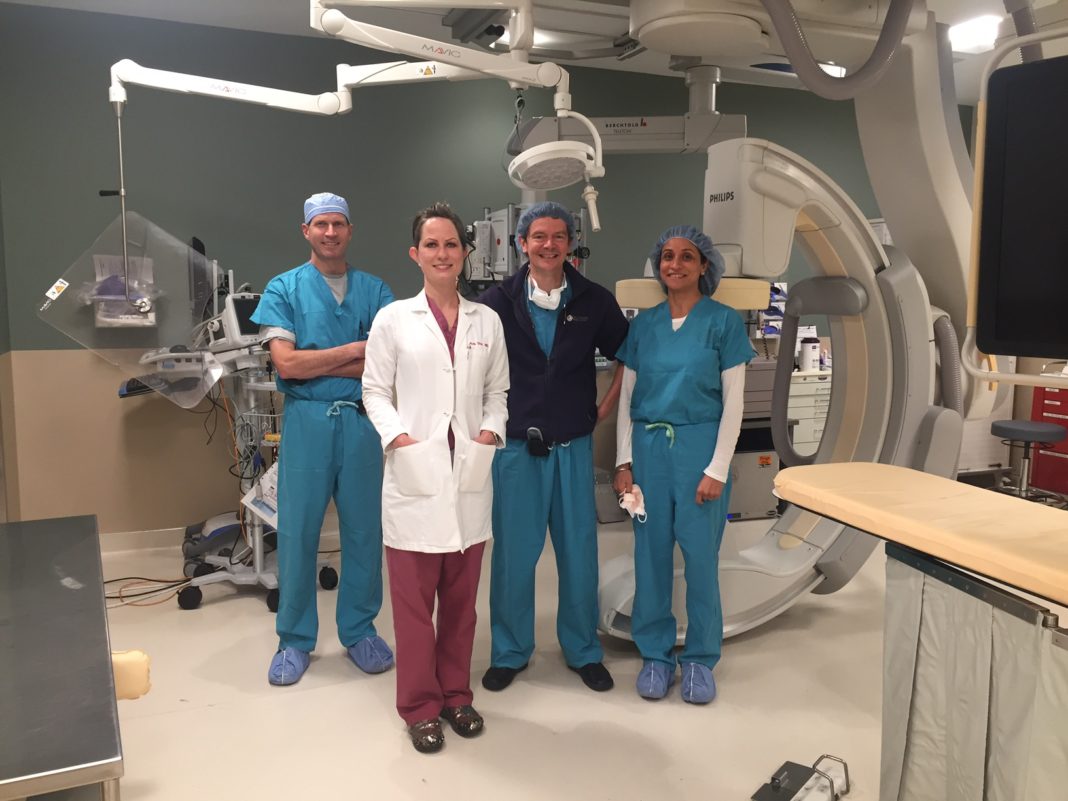
At South Sound Radiology, interventional radiologists like Dr. Boz work alongside diagnostic radiologists to offer support to multiple hospitals and medical centers around the region. Their service to patients like Cathy Obrien can make all the difference in emergency or trauma situations.
The difference between interventional and diagnostic radiologists is, while diagnostic radiology is generally non-invasive and used to detect problems, interventional radiology employs cutting edge techniques for minimally invasive procedures that can both save lives and radically alter the quality of life for patients. These include balloon angioplasty (opening narrow or blocked blood vessels with a small balloon), embolization (the use of metal coils or other embolic substances to block blood through a vessel), and percutaneous drain insertions (the placement of tubes in different parts of the body to drain fluids) among others. Their service to patients in hospital settings has long been valued, but until recently, their services have been largely procedure-based, only.

Historically, interventional radiologists had little to do with patients before and after procedures, leaving the consultation and follow-up to other doctors, says South Sound Radiology’s Dr. Evert Vershuyl. “If you were to seek out a provider, you would not have an environment where you could sit down in their office and learn enough to make an informed decision about which direction to go,” he says. “That was not available at all until we developed it at St. Peter’s.”
Now, through the Interventional Radiology Clinic, interventional radiologists work with neurosurgeons, neurologists and other medical staff to treat patients. “We’re familiar with all of the imaging techniques and we come up with a plan of attack for a certain procedure,” says Vershuyl.
Both patients and physicians have responded positively to the clinic. “Patients love it. We’re able to inform them of all the things we’re planning to do and tell them what they’re options are,” he says. “They’re getting better care. The providers that send us patients are freed from the burden of having to do all the follow-up.”
He cites two procedures that change the quality of life for patients in different ways. The first is kyphoplasty, the process of inserting cement into spinal compression fractures, a common problem among the elderly. “No other fracture would be left alone to heal on its own, but the traditional therapy has been rest, pain medication and maybe a brace,” says Vershuyl. “For older patients, that’s one of the worst things you can do. The side effects include blood clots in their legs or pneumonia.”
Kyphoplasty relieves the pain almost immediately and allows patients much greater mobility. “If we can get them into our clinic early, we’re able to fix that problem with a high degree of certainty,” says Vershuyl. “They’ll have a better quality of life without pain and without narcotics.”
Among young women, fibroid disease is a common problem and although most fibroid tumors are benign, they can still cause bleeding and other problems. Historically, the most common solution was a hysterectomy, an incredibly invasive procedure that left patients feeling diminished and required a five to six-week recovery period. Now, interventional radiologists can embolize the tumors and stop the bleeding, allowing patients to recover in seven to ten days. “It’s an alternative that people should at least consider,” says Vershuyl.
Cathy Obrien needs no further convincing of IR’s value. These days she’s gotten her strength back and her primary care doctor is tracking her progress. “I’ve had no further bleeding and my blood pressure is fine,” she says. “I’m grateful to Dr. Boz, to Providence and to God for getting me to the other side of this. I look around and during this wonderful summer we’re having, life is even more precious.”
For more information about South Sound Radiology, visit www.southsoundradiology.com or call 360-493-4600 for the imaging center.